Summary
In Germany, more than 5 million patients suffer from chronic kidney disease (CKD) - most of them without knowing it - and about 100,000 require renal replacement therapy in the form of dialysis or transplantation. CKD can result from systemic diseases such as diabetes mellitus, arterial hypertension, or immune disorders, as well as from primarily intrarenal causes such as primary glomerular disease, glomerular and interstitial inflammation, inherited tubular transport defects, or polycystic kidney disease. Regardless of which cell types are primarily affected, the tubular system and interstitial cells are critically involved in many of these disease processes and tubular atrophy and interstitial fibrosis are hallmarks of CKD progression.
In its first funding period, the CRC 1350 investigated the diverse functions and interplay of tubular epithelia and interstitial cells. We have gained important insights into pathomechanisms in several monogenic diseases, identified genetic risk factors in multifactorial kidney diseases, studied function and malfunction of interstitial cells, interstitial inflammation and fibrosis, and investigated damage memory and the consequences of hypoxia. For example, a team of CRC researchers uncovered the importance of TMEM16A (Ano1) chloride channels for cyst growth, confirmed the mechanism in animal models, demonstrated the efficacy of inhibitors of these channels, and finally established an ex vivo model to test the effects in human cystic kidney tissue to develop strategies for treatment of polycystic kidney patients.
For the next funding period, the overall goal is to further deepen our knowledge of the (patho ) physiology of the tubular system and the renal interstitium, with a focus on developing new diagnostic and therapeutic strategies.
To achieve this ambitious goal, we will incorporate further signaling pathways, new state-of-the-art methods, innovative models and analysis strategies into our research concept. For this, the transformation of CRC 1350 into TRR 374 is an important prerequisite, as this is the best way to achieve the necessary development. The research team will be further strengthened by the inclusion of outstanding (clinician) scientists, translational research projects and advanced data analysis. As TRR 374, we are well-positioned to shape nephrology research and to train the renal researchers and clinicians of the future.
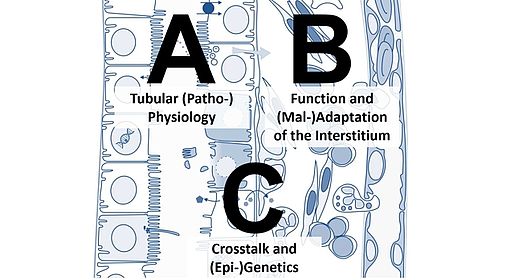
“Localization” of the projects within the tubulo-interstitium.
The focus of the projects of Research Area A is on the function of the tubular epithelium, on epithelial mechanisms of cyst formation and transport-related pathophysiology. Research Area B addresses the manifold functions of interstitial cells and their role in (mal-) adaptive processes. Research Area C studies processes involving both tubular cells and interstitial cells as well as the complex interaction between both.
MISSION
"Interdisciplinary kidney research to advance understanding of disease mechanisms and develop new therapeutic concepts"
Contact:
Dr. Michaela Kritzenberger
Email
Tel.: ++49 (0)941/943-2885